|
VIGsnfcomps.com utilizes data from Form CMS 2540-96 of the Healthcare Cost Report Information System (HCRIS) cost reports filed with Centers for Medicare and Medicaid Services (CMS). All Content provided by third party users in connection with this Website is the responsibility of the person or entity providing such Content. THE CONTENT FOUND ON THE WEBSITE MAY NOT BE APPROPRIATE OR SATISFACTORY FOR YOUR USE, AND YOU SHOULD VERIFY ALL CONTENT BEFORE RELYING ON IT. THE MATERIALS PROVIDED AT THIS SITE ARE PROVIDED "AS IS" WITHOUT ANY WARRANTIES OF ANY KIND INCLUDING WARRANTIES OF MERCHANTABILITY, FITNESS FOR A PARTICULAR PURPOSE, OR NON-INFRINGEMENT OF INTELLECTUAL PROPERTY. The worksheets used for VIG SNF Comps are:
The Paperwork Reduction Act of 1980 establishes the requirement that the private sector be informed as to why information is collected and what the information is used for by the government. In accordance with §1815(a) and §1861(v)(1)(A)(ii) of the Social Security Act, providers of service participating in the Medicare program are required to submit annual information to achieve settlement of costs for health care services rendered to Medicare beneficiaries. Also, 42 CFR 413.20(b) requires cost reports from providers on an annual basis. Besides determining program reimbursement, the data submitted on the cost report supports management of the Federal programs, e.g., data extraction in developing cost limits and SNF prospective payment rates. In completing Form HCFA-2540S-87, the information reported must conform to the requirements and principles set forth in the Provider Reimbursement Manual, Part I (HCFA Pub. 15-I). The instructions contained in this chapter are effective for cost reporting periods beginning on or after October 1, 1986. These instructions apply to the entire cost report (Form HCFA-2540S), as well as to the input sheets which do not require the mathematical calculations needed to complete the cost report. The line numbers on the input sheets are the same line numbers reflecting the same data in the cost report. You may complete only the input sheets; your intermediary then prepares your cost report and returns a copy to you. COMPLETE ONLY THE COST REPORT OR THE INPUT SHEETS. In lieu of submitting hard copy input sheets (which contain only the data needed to prepare the cost report) or a hard copy cost report, you may obtain from your intermediary a computer software package which enables you to computerize your cost report. If you have the appropriate computer equipment, please contact your intermediary for more information. HCFA prefers to receive cost reports in disc or tape format rather than in hard copy. (NOTE: the computer software package and instructions are furnished at no cost to you.) With respect to the computer software, its use essentially requires only the data on the input sheets to be entered into the system. The computer program develops the cost report from that data. The option to file less than a full cost report as prescribed in HCFA Pub. 15-1 §2414(B) is still available to those SNFs electing prospective payment. Cost reports are due on or before the last day of the third month following the close of the period covered by the report. A 30-day extension of the due date may, for good cause, be granted by the intermediary, after first obtaining the approval of the Health Care Financing Administration. The cost report from a provider which voluntarily or involuntarily ceases to participate in the health insurance program or experiences a change of ownership is due no later than 45 days following the effective date of the termination of the provider agreement or change of ownership. There are no provisions for an extension of the cost report due date with respect to termination of the provider agreement or change of ownership. If a provider does not furnish any covered services to Medicare beneficiaries during a cost reporting period, it is not required to submit a full cost report. It must, however, submit an abbreviated cost report as prescribed in chapter 1, §110A. NOTE:
Supplemental worksheets are provided on an as needed basis depending on the complexity of the skilled nursing facility. Not all supplemental worksheets are needed by all skilled nursing facilities. Following are a few examples of conditions for which supplemental worksheets are needed:
If you participate in either title V or XIX, you may substitute the lines and columns used for title XVIII for reporting these programs. These forms include the combination method of cost finding which provides for combining certain general service cost centers into four cost groups located on Worksheet B and B-1. Once the costs of a general service cost center have been grouped and allocated, those cost centers are considered "closed". Being "closed", they do not receive any of the costs that are subsequently allocated from the remaining general service cost centers. After all costs of the general service cost centers have been allocated to the remaining cost centers, the total costs of these remaining cost centers are further distributed to the departmental classification to which they pertain, e.g., skilled nursing facility inpatient, skilled nursing facility intermediate care. In completing the worksheets, reductions in expenses must always be shown in parentheses ( ). Cost reports are due on or before the last day of the third month following the close of the period covered by the report. A 30-day extension of the due date may, for good cause, be granted by the intermediary after first obtaining HCFA approval. The cost report from a provider which voluntarily or involuntarily ceases to participate in the health insurance program or experiences a change of ownership is due no lather than 45 days following the effective date of the termination of the provider agreement or change of ownership. There are no provisions for an extension of the cost report due date with respect to termination. If you do not furnish any covered services to Medicare beneficiaries during a cost reporting period, you are not required to submit a full cost report. You must, however, submit an abbreviated cost report as prescribed in §110A. ROUNDING STANDARDS FOR FRACTIONAL COMPUTATIONS Throughout the Medicare cost report, required computations result in the use of fractions. The following rounding standards must be employed for such computation:
-- Averages -- Full Time Equivalent Employees -- Per diems
If a residual exists as a result of computing costs using a fraction, the amount remaining is added to the largest amount resulting from the computation. For example, in cost finding, a unit cost multiplier is applied to the statistics in determining costs. After rounding each computation, the sum of the allocation may be more or less than the total cost being allocated. This residual is adjusted to the largest amount resulting from the allocation so that the sum of the allocated amounts equals the amount being allocated.
This worksheet checklist identifies each worksheet that is completed as a part of this cost report. Worksheets which are not completed because they are not applicable to the provider are not required to be submitted. The cost report consists of core worksheets (Form HCFA-2540-92) and supplemental worksheets (A-8-1 through M-4). With few exceptions, the core worksheets are generally applicable to most SNFs filing a Medicare cost report. In some instances, a part of a core worksheet may not be applicable in an individual reporting situation. Supplemental worksheets are applicable to unique circumstances in individual reporting situations. Some worksheets (both core and supplemental) are used only one time regardless of the cost reporting situation. Other worksheets may be used more than one time in a single cost report depending upon the individual circumstances of the SNF. Worksheet S-1, Part I - Worksheets Used Only One Time in Cost Report.--Indicate in the appropriate space whether the worksheet is submitted on a HCFA form, is computer prepared, or is not applicable. Worksheet S-1, Part II - Worksheets That May Be Used More Than One Time in Cost Report.--A separate Worksheets S-1, Part II, must be filed for each health care program (title V, XVIII and XIX) for which the cost report is applicable. Indicate, in the appropriate spaces, each component of the health care complex for which a worksheet is included in the cost report and whether the worksheet is submitted on a HCFA form, is computer prepared, or not applicable.
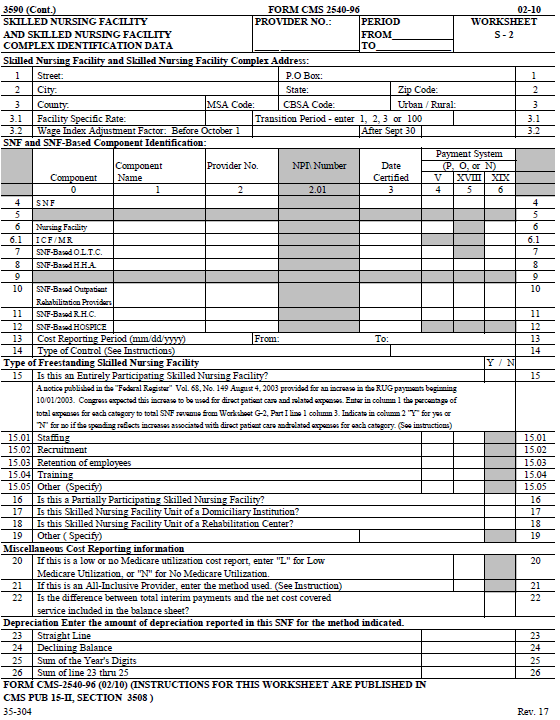
The information required on this worksheet is needed to properly identify the provider. Enter the provider identification number and the date certified. Lines 1 through 1.02.--Enter the name, address, and county of the skilled nursing facility. The following definitions apply when completing these cost reporting forms. Enter the component name, provider number, date certified, and payment system on the applicable line description. Line 2.--This is an institution which meets the requirements of §1819(b)(c)(d) of title XVIII - Health Insurance for the Aged and Disabled of the Social Security Act. Line 3.--This is a portion of an SNF which has been issued a separate identification number and which meets the requirements of §1919 of title XIX. Line 5.--This is a distinct part and separately certified component of an SNF which meets the requirements of §1861(o) of title XVIII - Health Insurance for the Aged and Disabled of the Social Security Act. Line 6.--This is a distinct part and separately certified component of a skilled nursing facility which meets the requirements of §1861(cc) of title XVIII - Health Insurance for the Aged and Disabled of the Social Security Act. Line 7.--This is a distinct part and separately certified component of a skilled nursing facility which meets the requirements of §1861(ff) of title XVIII - Health Insurance for the Aged and Disabled of the Social Security Act. Line 8.--Enter the inclusive dates covered by this cost report. In accordance with 42 CFR 413.20(b), you are required to submit periodic reports of operations which generally cover a consecutive 12-month period of operations. (See HCFA PUB 15-II, chapter 1 for situations when a short period cost report may be filed.) Line 9.--Enter a number from the list below which indicates the type of ownership or auspices under which the SNF is conducted.
Lines 10 through 17.--These lines provide for furnishing certain information concerning the provider. All applicable items must be completed. Line 16.--Enter ONLY A, B, or E for the all-inclusive method, or leave it BLANK. Do not enter an "N". Lines 18 through 25.--These lines provide for furnishing certain information concerning depreciation. All applicable items must be completed. (See HCFA Pub. 15-I, chapter 1, regarding depreciation.) Lines 18, 19, and 20.--Indicate, on the appropriate lines, the amount of depreciation claimed under each method of depreciation used by the SNF during the cost reporting period. Line 21.--The total depreciation shown on this line may not equal the amount shown on lines 1 and/or 2 on the Trial Balance of Expenses Worksheet, but represents the amount of depreciation included in costs on Worksheet A, column 7. Lines 23 through 27.--Indicate a "Yes" or "No" answer to each question on these lines.
Lines 28 through 33.--Indicate a "Yes" or "No" answer, where applicable, to each component and type of service that qualifies for the exception. If you are a provider (public or non public) that qualifies for an exemption from the application of the lower of cost or charges (as explained in 42 CFR 413.13(f)), indicate the component and the appropriate services that qualify for this exemption. Subscript lines 28 through 33 as required for additional component(s). Line 34.--Indicate whether the provider participated in the NHCMQ demonstration during the cost reporting period. All NHCMQ demonstration participants must file Form HCFA 2540-92, including facilities reporting less than 1,500 program days which would otherwise be allowed to utilize the Form HCFA 2540S-87. Only facilities in Kansas, Maine, Mississippi, New York, South Dakota, and Texas are eligible to participate in the NHCMQ demonstration.
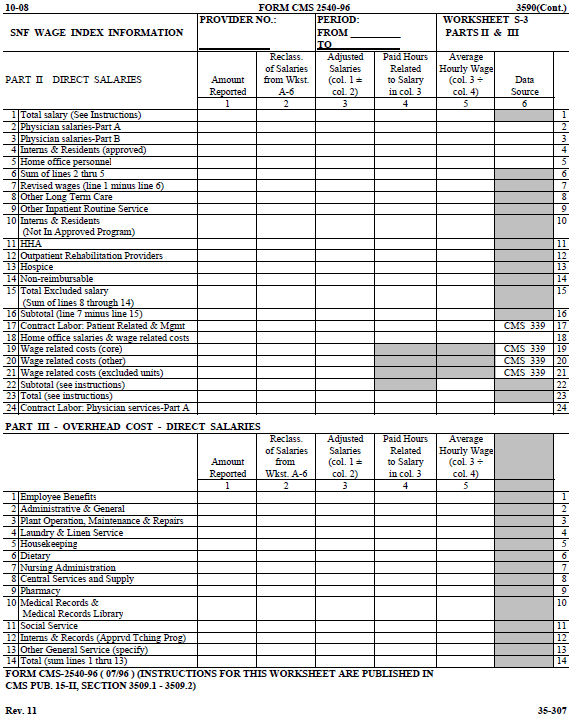
In accordance with 42 CFR 413.60(a), 42 CFR 413.24(a), and 42 CFR 413.40(c), you are required to maintain statistical records for proper determination of costs payable under the Medicare program. The statistics reported on this worksheet pertain to SNF, nursing facility, other long term care services, HHA, CORF, and CMHC. The data to be maintained, depending on the services provided by the component, include the number of beds available, the number of admissions, the number of discharges, the average length of stay, the number of inpatient days, the bed days available, and FTEs. Column Descriptions Column 1.--Enter on the appropriate line the statistics related to the inpatients of the facility (SNF on line 1, nursing facility on line 2, or SNF-based other long term care facility on line 3). Column 2.--Enter the total bed days available. Bed days are computed by multiplying the number of beds available throughout the period by the number of days in the reporting period. If there is an increase or decrease in the number of beds available during the period, multiply the number of beds available for each part of the cost reporting period by the number of days for which that number of beds was available. Columns 3 through 6.--Enter the number of inpatient days for each component by program. Column 7.--Enter the total number of inpatient days to include all classes of patients for each component. Columns 8 through 11.--Enter the number of discharges, including deaths (excluding newborn and DOAs), for each component by program. A patient discharge, including death, is a formal release of a patient. Column 12.--Enter the number of discharges (including deaths) for all classes of patients for each component. Columns 13 through 16.--The average length of stay is calculated as follows:
Columns 17 through 21.--Enter the number of admissions (from your records) for each component by program. Columns 22 and 23.--The average number of employees (full-time equivalent) for the period may be determined either on a quarterly or semiannual basis. When quarterly data are used, add the total number of hours worked by all employees on the first payroll at the beginning of each quarter and divide the sum by four times the number of hours in the standard work period. When semiannual data are used, add the total number of hours worked by all employees on the first payroll of the first and seventh months of the period, and divide this sum by two times the number of hours in the standard work period. Enter the average number of paid employees in column 22 and the average number of nonpaid workers in column 23 for each component, as applicable.
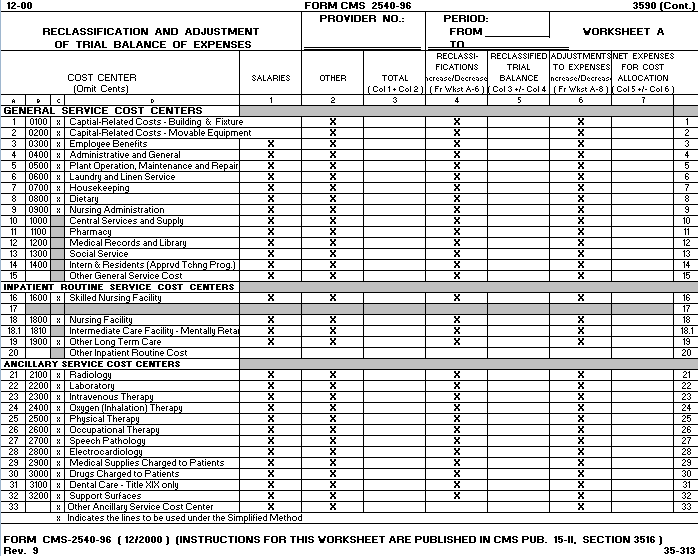
In accordance with 42 CFR 413.20, the methods of determining costs payable under title XVIII involve making use of data available from the institution’s basic accounts, as usually maintained, to arrive at equitable and proper payment for services. Worksheet A provides for recording the trial balance of expense accounts from your accounting books and records. It also provides for the necessary reclassifications and adjustments to certain accounts. The cost centers on this worksheet are listed in a manner which facilitates the transfer of the various cost center data to the cost finding worksheets (i.e., on Worksheets A, B, C, and D, the line numbers are consistent). All of the cost centers listed do not apply to all providers using these forms. Do not include on this worksheet items not claimed in the cost report because they conflict with the regulations, manuals, or instructions but which you wish nevertheless to claim and contest. Enter amounts on the appropriate settlement worksheet (Worksheet E, Part I, line 39; Worksheet E, Part II, line 32; Worksheet E, Part III, line 39; Supplemental Worksheet H-6, Part II, line 25; Supplemental Worksheet J-3, line 20; or Supplemental Worksheet M-3, line 31). If the cost elements of a cost center are separately maintained on your books, you must maintain a reconciliation of the costs per the accounting books and records to those on this worksheet. The reconciliation is subject to review by the intermediary. Standard (i.e., preprinted) HCFA line numbers and cost center descriptions cannot be changed. If you need to use additional or different cost center descriptions, you may do so by adding additional lines to the cost report. When an added cost center description bears a logical relationship to a standard line description, the added label must be inserted immediately after the related standard line description. Identify the added line as a numeric (only) subscript of the immediately preceding line. That is, if two lines are added between lines 5 and 6, identify them as lines 5.01 and 5.02. If additional lines are added for general service cost centers, add corresponding columns for cost finding on, Worksheets B and B-1 and Supplemental Worksheets J-1 and M-1. Submit the working trial balance of the facility with the cost report. A working trial balance is a listing of the balances of the accounts in the general ledger to which adjustments are appended in supplementary columns and used as a basic summary for financial statements. Columns 1, 2, and 3.--The expenses listed in these columns must be in accordance with your accounting books and records. List on the appropriate lines in columns 1, 2, and 3 the total expenses incurred during the cost reporting period. Detail the expense between salaries (column 1) and other than salaries (column 2). The sum of columns 1 and 2 must equal column 3. Record any needed reclassification and/or adjustments in columns 4 and 6, as appropriate. Column 4.--Enter any reclassification among the cost center expenses in column 3 which are needed to effect proper cost allocation. Worksheet A-6 reflects the reclassification affecting the cost center expenses. This worksheet need not be completed by all providers but must be completed only to the extent that the reclassification are needed and appropriate in the particular provider’s circumstances. Show reductions to expenses in parentheses ( ). The net total of the entries in column 4 must equal zero on line 63. Column 5.--Adjust the amounts entered in column 3 by the amounts in column 4 (increase or decrease) and extend the net balances to column 5. The total of column 5 must equal the total of column 3 on line 63. Column 6.--Enter on the appropriate lines in column 6 of Worksheet A the amounts of any adjustments to expenses indicated on Worksheet A-8, column 2. The total on Worksheet A, column 6, line 63 must equal Worksheet A-8, column 2, line 32. Column 7.--Adjust the amounts in column 5 by the amounts in column 6 (increases or decreases) and extend the net balances to column 7. Transfer the amounts in column 7 to the appropriate lines on Schedule B, Part I, column 0. Line Descriptions The trial balance of expenses is broken down into general service, inpatient routine service, ancillary service, outpatient service, other reimbursable, special purpose, and nonreimbursable cost center categories to facilitate the transfer of costs to the various worksheets. For example, the categories "Ancillary Cost Centers" and "Outpatient Cost Centers" appear on Worksheet D using the same line numbers as on Worksheet A. NOTE: The category titles do not have line numbers. Only cost centers, data items, and totals have line numbers. Lines 1 and 2.-These cost centers include depreciation, leases, and rentals for the use of facilities and/or equipment, interest incurred in acquiring land or depreciable assets used for patient care, insurance on depreciable assets used for patient care, and taxes on land or depreciable assets used for patient care. Do not include in these cost centers costs incurred for the repair or maintenance of equipment or facilities, amounts included in rentals or lease payments for repair and/or maintenance agreements, interest expense incurred to borrow working capital or for any purpose other than the acquisition of land or depreciable assets used for patient care, general liability insurance or any other form of insurance to provide protection other than the replacement of depreciable assets, or taxes other than those assessed on the basis of some valuation of land or depreciable assets used for patient care. Many providers incur costs applicable to services, facilities, and supplies furnished to the provider by organizations related to the provider by common ownership or control. Section 42 CFR 413.17 and HCFA Pub. 15-I, chapter 10, require that the reimbursable cost of the provider include the costs for these items at the cost to the supplying organization (unless the exception provided in 42 CFR 413.17(d) and HCFA Pub. 15-I, §1010 is applicable). However, if the price in the open market for comparable services, facilities, or supplies is lower than the cost to the supplier, the allowable cost to you may not exceed the market price. The rationale behind this policy is that when you are dealing with a related organization, you are essentially dealing with yourself. Therefore, your costs are considered equal to the cost to the related organization. If you include on the cost report costs incurred by a related organization, the nature of the costs (i.e., capital-related or operating costs) do not change. Treat capital-related costs incurred by a related organization as your capital-related costs. However, if the price in the open market for comparable services, facilities, or supplies is lower than the cost to the supplying related organization, your allowable cost may not exceed the market price. Unless the services, facilities, or supplies are otherwise considered capital-related cost, no part of the market price is considered capital-related cost. Also, if the exception in 42 CFR 413.17(d) and HCFA Pub.15-I, §1010 applies, no part of the cost to you of the services, facilities, or supplies is considered capital-related cost unless the services, facilities, or supplies are otherwise considered capital-related. If the supplying organization is not related to you within the meaning of 42 CFR 413.17, no part of the charge to you may be considered a capital-related cost (unless the services, facilities, or supplies are capital-related in nature) unless: o The capital-related equipment is leased or rented by you; o The capital-related equipment is located on your premises or is located offsite and is on real estate owned, leased, or rented by you; and o The capital-related portion of the charge is separately specified in the charge to you. Under certain circumstances, costs associated with minor equipment may be considered capital-related costs. HCFA Pub. 15-I, §106 discusses methods for writing off the cost of minor equipment. Three methods are presented in that section. Amounts treated as expenses under method (a) are not capital-related costs because they are treated as operating expenses. Amounts included in expense under method (b) are capital-related costs because such amounts represent the amortization of the cost of tangible assets over a projected useful life. Amounts determined under method (c) are capital-related costs because method (c) is a method of depreciation. Line 9.--This cost center normally includes only the cost of nursing administration. The salary cost of direct nursing services (including the salary cost of nurses who render direct service in more than one patient care area) are directly assigned to the various patient care cost centers in which the services were rendered. Direct nursing services include gross salaries and wages of head nurses, registered nurses, licensed practical and vocational nurses, aides, orderlies, and ward clerks. However, if your accounting system fails to specifically identify all direct nursing services to the applicable patient care cost centers, then the salary cost of all direct nursing service is included in this cost center. Line 12.--This cost center includes the direct cost of the medical records cost center including the medical records library. The general library and the medical library must not be included in this cost center. Report them in the administrative and general cost center. Line 14.--Use this line to record the cost of intern and residents if the SNF maintains an intern and residents program. Lines 16 through 19.--These lines are for the inpatient routine service cost centers. Line 18.--This cost center accumulates the direct costs incurred in maintaining long term care services not specifically required to be included in other cost centers. A long term care unit refers to a unit where the average length of stay for all patients is 25 days or more. The beds in this unit are not certified for titles V, XVIII, or XIX. Lines 21 through 32.--These lines are for the ancillary cost centers.
Lines 34 and 35.--These lines are for outpatient cost centers. Lines 36 through 49.--These lines are for other reimbursable cost centers. Lines 36 through 46.--These lines are provided to accumulate costs which are specific to HHA services. Line 36.--This cost center accumulates the direct costs attributable to HHA administrative and general costs. Provider-based HHAs are operated and managed in a variety of ways within the context of the health care complexes of which they are components. In some instances, there are discrete management and administrative functions pertaining to the HHA, the cost of which is readily identifiable from the books and records. In other instances, the administration and management of the provider-based HHA is integrated with the administration and management of the health care complex to such an extent that the cost of administration and management of the home health agency can be neither identified nor derived from the books and records of the health care complex. In other instances, the cost of administration and management of the HHA is integrated with the administration and management of the health care complex, but the cost of the HHA administration and management can be derived through cost finding. However, in most cases, even where the cost of HHA administration and management can be either identified or derived, the extent to which the costs are applicable to the services furnished by the provider-based HHA is not readily identifiable. Even when the costs of administration and management of a provider-based HHA can be identified or derived, such costs do not generally include all of the general service costs (i.e., overhead costs) applicable to the HHA. Therefore, allocation of general service costs through cost finding is necessary for the determination of the full costs of the provider-based HHA. If the provider-based HHA can identify discrete management and administrative costs from its books and records, include these costs on line 36. Similar situations occur for services furnished by the provider-based HHA. For example, in some instances, physical therapy services are furnished by a discrete HHA physical therapy department. In other instances, physical therapy services are furnished to the patients of the provider-based HHA by an integrated physical therapy department of a SNF health care complex in such a manner that the direct costs of furnishing the physical therapy services to the patients of the provider-based HHA cannot be readily identified or derived. In still other instances, physical therapy services are furnished to patients of the provider-based HHA in an integrated physical therapy department of an SNF health care complex in such a manner that the costs of physical therapy services furnished to patients of the provider-based HHA can be readily identified or derived. If you maintain a separate therapy department for the HHA apart from the SNF therapy department furnishing services to other patients of the health care complex or are able to reclassify costs from an integrated therapy department to an HHA-therapy cost center, then make a reclassification entry on Worksheet A-6 to the appropriate HHA therapy cost center. Make a similar reclassification to the appropriate line for other ancillaries when the HHA costs are readily identifiable. NOTE: This cost report provides separate HHA cost centers for all therapy services. If services are provided to HHA patients from a shared SNF ancillary cost center, make the cost allocation on Worksheet B. Line 37.--This cost center includes the direct patient care costs incurred for skilled nursing care to patients who are normally at their place of residence. Lines 38 through 40.--These lines provide for Physical Therapy - HHA, Occupational Therapy - HHA, and Speech Pathology - HHA cost centers. These are new cost centers which provide for these therapy services when only HHA patients are serviced from them. Line 41.--This cost center includes the direct patient care cost incurred for counseling and assessment activities which contribute meaningfully to the treatment of a patient§s condition within the context of home health care. Line 42.--This cost center includes the direct patient care costs incurred for services performed by specially trained personnel who assist individuals in carrying out physicians§ instructions under an established plan of care. Line 43.--Enter the cost of durable medical equipment (DME) rented to home health patients. (See HCFA Pub. 11, §206.) Line 44.--Enter the cost of DME sold to home health patients. Line 45.--Enter the cost of a home delivered meals program. This service is not reimbursable under title XVIII. However, it may be reimbursable by a State program, and, as such, identify the cost for that purpose. Line 46.--This cost center includes the direct costs of noncovered home health services for Medicare cost reporting purposes. Noncovered services include homemaker services, home dialysis aide services, private duty nursing, health promotion activities, and day care programs. Line 47.--This cost center accumulates the direct costs attributable to a comprehensive outpatient rehabilitation facility (CORF). Direct costs normally include such cost categories as are listed on Supplemental Worksheet J-1, lines 1 through 15. Line 49.--This cost center accumulates the direct costs attributable to a community mental health center (CMHC). Direct costs normally include such cost categories as are listed on Supplemental Worksheet M-1, lines 1 through 15. Lines 50 through 54.--These lines are for special purpose cost centers. Line 50.--This cost center includes the costs of malpractice insurance premiums and self insurance fund contributions. Also, include the cost if you pay uninsured malpractice losses incurred either through deductible or coinsurance provisions, or as a result of an award in excess of reasonable coverage limits, or as a governmental provider. For cost reporting periods beginning on or after May 1, 1986, reclassify malpractice insurance expense to administrative and general expense and allocate to the revenue producing cost centers on Worksheet B, Part I, based upon the recommended basis of allocation provided in Worksheet B-1. Line 52.--Only include utilization review costs of the SNF. Either reclassify or adjust all costs depending on the scope of the review. If the scope of the review covers all patients, reclassify all allowable costs in column 4 to administrative and general expenses (line 4). If the scope of the review covers only Medicare patients or Medicare, title V and title XIX patients, then (1) in column 4, reclassify to administrative and general expenses all allowable costs other than physician compensation and (2) deduct, in column 6, the compensation paid to the physicians for their personal services on the utilization review committee. Line 53.--This cost center accumulates the direct costs attributable to a hospice. Lines 57 through 62.--Use these lines to record the costs applicable to nonreimbursable cost centers to which general service costs apply. If additional lines are needed for nonreimbursable cost centers than those shown, add a subscript consisting of a numeric subscript code to one or more of these lines. The subscripted lines must be appropriately labeled to indicate the purpose for which they are being used. However, if the expense (direct and all applicable overhead) attributable to any nonallowable cost area is so insignificant as not to warrant establishment of a nonreimbursable cost center and the sum total of all such expenses is so insignificant as not to warrant the establishment of a composite nonreimbursable cost center, adjust these expenses on Worksheet A-8. (See HCFA Pub. 15-I, §2328.) Line 59.--Establish a nonreimbursable cost center to accumulate the cost incurred by the provider for services related to the physicians’ private practice. Examples of such costs include depreciation costs for the space occupied, movable equipment used by the physicians’ offices, administrative services, medical records, housekeeping, maintenance and repairs, operation of plant, drugs, medical supplies, and nursing services. This nonreimbursable cost center does not include costs applicable to services which benefit the general population or for direct patient services rendered by SNF-based physicians.
Part III - SNFs Reimbursed Under PPS 1620.3 Part III - SNF Reimbursed Under PPS.--Use this part to calculate reimbursement settlement under PPS for titles V, XVIII, and XIX services furnished by SNFs and NFs. Line 7.--The amount entered is the number of program days multiplied by the prospective payment rate or the routine service cost limit, whichever is less. NOTE: The rate on applicability due to flat rate is provided by the intermediary. Enter Medicare days from your records.
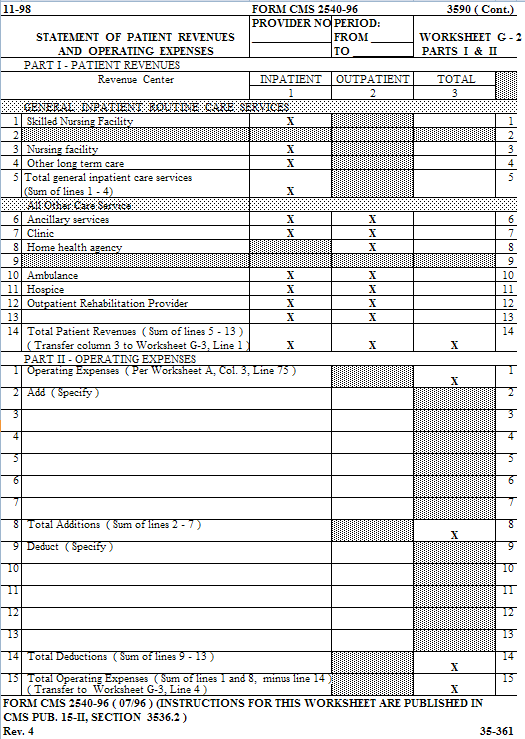
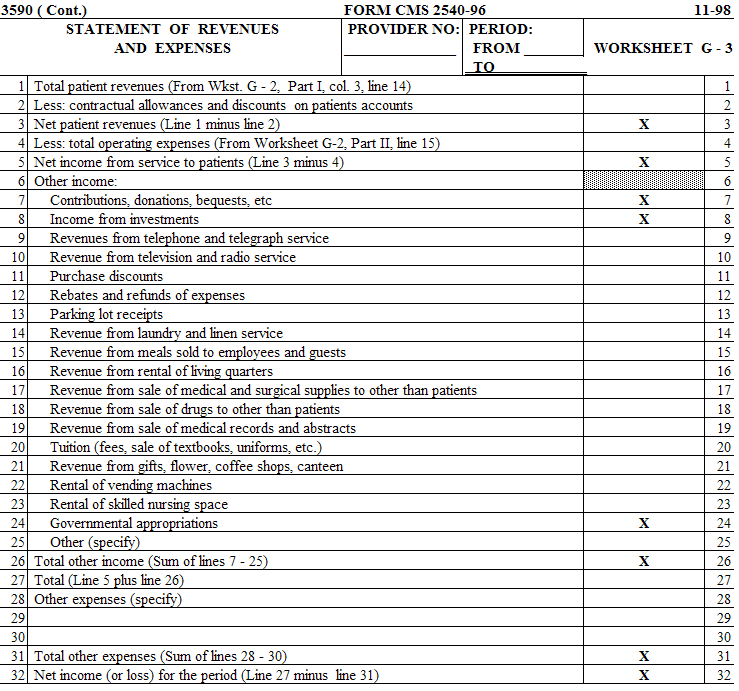
Worksheets G and G-1 are completed by all providers maintaining fund-type accounting records. Nonproprietary providers which do not maintain fund-type accounting records complete the General Fund columns only.
|
||||||||||||||||||||||||||